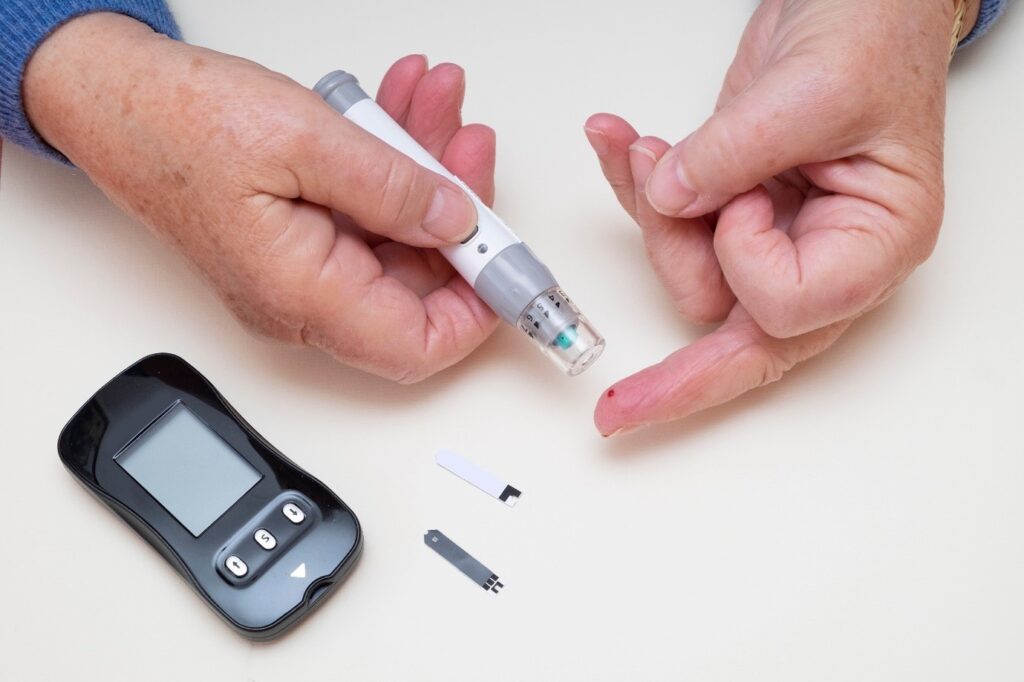
What is Type 2 diabetes?
It is a chronic condition that affects how the body regulates and uses sugar, also known as glucose.
This results in increased blood sugar levels, which can cause complications in the circulatory, nervous, and immune systems.
The condition primarily arises from two issues: the pancreas does not produce enough insulin, and the body’s cells become resistant to insulin, reducing glucose absorption.
What are the Causes and Mechanisms?
Insulin, a hormone produced by the pancreas, plays a crucial role in regulating the body’s glucose levels.
Normally, insulin helps move sugar from the bloodstream into the cells for energy.
In type 2 diabetes, the body’s cells—especially in muscle, fat, and the liver—become resistant to insulin, meaning sugar isn’t efficiently taken up by the cells.
Additionally, the pancreas eventually struggles to produce enough insulin to meet the body’s needs.
As a result, sugar accumulates in the bloodstream.
While the exact cause of type 2 diabetes is not fully understood, being overweight, having an inactive lifestyle, and genetic factors are significant contributors.
Risk Factors
Many factors increase the risk of developing type 2 diabetes, including:
- Weight: Being overweight, especially with abdominal fat, is a major risk factor.
- Inactivity: A sedentary lifestyle increases the risk.
- Family history: Having a parent or sibling with type 2 diabetes increases the likelihood.
- Age: Risk increases after age 35, particularly if combined with other risk factors.
- Race and ethnicity: Populations such as Black, Hispanic, Native American, Asian, and Pacific Islander have a higher risk.
- Prediabetes: High blood sugar levels, not yet at diabetic levels, can develop into type 2 diabetes if untreated.
- Other conditions: Polycystic ovary syndrome (PCOS), gestational diabetes, and high blood pressure are also linked to a higher risk.
Symptoms
Type 2 diabetes progresses slowly and may remain undetected for years. Common symptoms include:
- Increased thirst and frequent urination
- Hunger and unintended weight loss
- Fatigue and blurred vision
- Slow-healing sores and frequent infections
- Numbness or tingling in hands or feet
- Darkened skin, often around the neck or armpits
What are the Complications of Type 2 Diabetes?
If type 2 diabetes is left untreated, it may lead to complications, including:
- Heart and blood vessel disease: Elevated risk of heart disease, stroke, and high blood pressure.
- Nerve damage (neuropathy): Can lead to tingling, pain, or loss of feeling in the extremities.
- Kidney disease: Diabetes can cause kidney damage, potentially leading to kidney failure.
- Eye damage: Increased risk of cataracts, glaucoma, and diabetic retinopathy, which can lead to blindness.
- Skin issues: Increased risk of bacterial and fungal infections.
- Poor healing: Cuts and sores may heal slowly, increasing the risk of serious infection.
- Hearing problems and sleep apnea: Diabetes can contribute to hearing loss and is commonly associated with sleep apnea.
- Dementia: Poor blood sugar control can increase the risk of cognitive decline and Alzheimer’s disease.
How is it Diagnosed?
Type 2 diabetes is diagnosed through blood tests. The most common test is the A1C test, which measures blood sugar levels over the past two to three months:
- A1C below 5.7% is normal.
- A1C between 5.7% and 6.4% indicates prediabetes.
- A diagnosis of diabetes is confirmed when an A1C level of 6.5% or higher is observed on two separate tests.A1C of 6.5% or higher on two separate tests indicates diabetes.
Other tests include:
- Fasting blood sugar: A level of 126 mg/dL or higher indicates diabetes.
- Oral glucose tolerance test: A reading of 200 mg/dL or higher two hours after testing indicates diabetes.
How is it Prevented?
Lifestyle changes can help prevent type 2 diabetes, especially for those with prediabetes.
Key prevention strategies include:
- Healthy eating: Prioritize fruits, vegetables, whole grains, and lean proteins, while reducing intake of sugars and refined carbohydrates.
- Physical activity: Aim for at least 150 minutes of moderate exercise each week, such as walking, swimming, or cycling.
- Weight management: Losing 5-10% of body weight can significantly reduce the risk of developing diabetes.
- Avoid prolonged inactivity: Stand or move around every 30 minutes to reduce the risk of diabetes.
How is it Treated?
While there is no cure for type 2 diabetes, it can be managed with lifestyle changes and, if necessary, medications. Treatment includes:
- Healthy Eating: A balanced diet focused on whole grains, vegetables, and lean proteins, with regular meal timing and portion control.
- Physical Activity: A combination of aerobic exercise and resistance training can help manage blood sugar and improve insulin sensitivity.
- Weight Loss: Even modest weight loss (5-10%) can improve blood sugar control, cholesterol, and blood pressure.
- Blood Sugar Monitoring: Regular testing of blood sugar levels is essential to track how well the condition is being managed.
- Medications: If lifestyle changes are not enough to control blood sugar, medications may be prescribed. Common drugs include:
- Metformin: The first-line treatment, which reduces glucose production in the liver and improves insulin sensitivity.
- Sulfonylureas (e.g., glipizide): Help the pancreas release more insulin.
- GLP-1 receptor agonists (e.g., liraglutide): Slow digestion, improve insulin sensitivity, and often aid in weight loss.
- SGLT2 inhibitors (e.g., empagliflozin): Help the kidneys filter out glucose from the bloodstream.
- Insulin Therapy: Some people with type 2 diabetes require insulin therapy. Insulin injections help maintain stable blood sugar levels, especially if other medications and lifestyle changes aren’t enough.
- Weight-loss Surgery: For those with severe obesity, weight-loss surgery (bariatric surgery) can help achieve significant weight loss and improve diabetes management.
Special Considerations
- Pregnancy: Pregnant individuals with type 2 diabetes may need to adjust their treatment plan, and some may require insulin therapy to control blood sugar.
- Mental Health: Managing type 2 diabetes can be emotionally challenging. Psychological support, stress management, and coping strategies are essential for overall well-being.
Monitoring and Long-term Management
Regular blood sugar monitoring is vital in managing type 2 diabetes. Patients should collaborate with their healthcare team to establish personalized goals for A1C levels and other health metrics. Continuous glucose monitors (CGMs) provide real-time tracking of blood sugar, offering more accurate control and notifying patients when their levels are too high or low.
By focusing on lifestyle changes, regular medical check-ups, and appropriate use of medications, people with type 2 diabetes can effectively manage their condition and reduce the risk of complications.
Experience compassionate care and advanced treatments at Prime Care Hospitals – Your health, our priority. Schedule your appointment today!